Prior Authorization Decoded
Prior authorization is not an insurer’s way of saying no. It’s a process to determine medical necessity. Now you’re going to understand how it works so you can work it.
Prior authorization is not an insurer’s way of saying no. It’s a process to determine medical necessity. Now you’re going to understand how it works so you can work it.
Quick recap from Module 2: You now understand how insurance plans work, what your rights are when plans deny coverage, and how to negotiate with your provider. In this module, you’ll focus on one specific gatekeeper process: prior authorization. What it is, why plans use it, and exactly what you can do if PA gets in your way.
James got a call from his doctor’s office: “We need to submit a prior authorization request for your GLP-1.” His first thought was: here we go, insurance is going to deny me. But I want to reframe what’s actually happening—for James and for you.
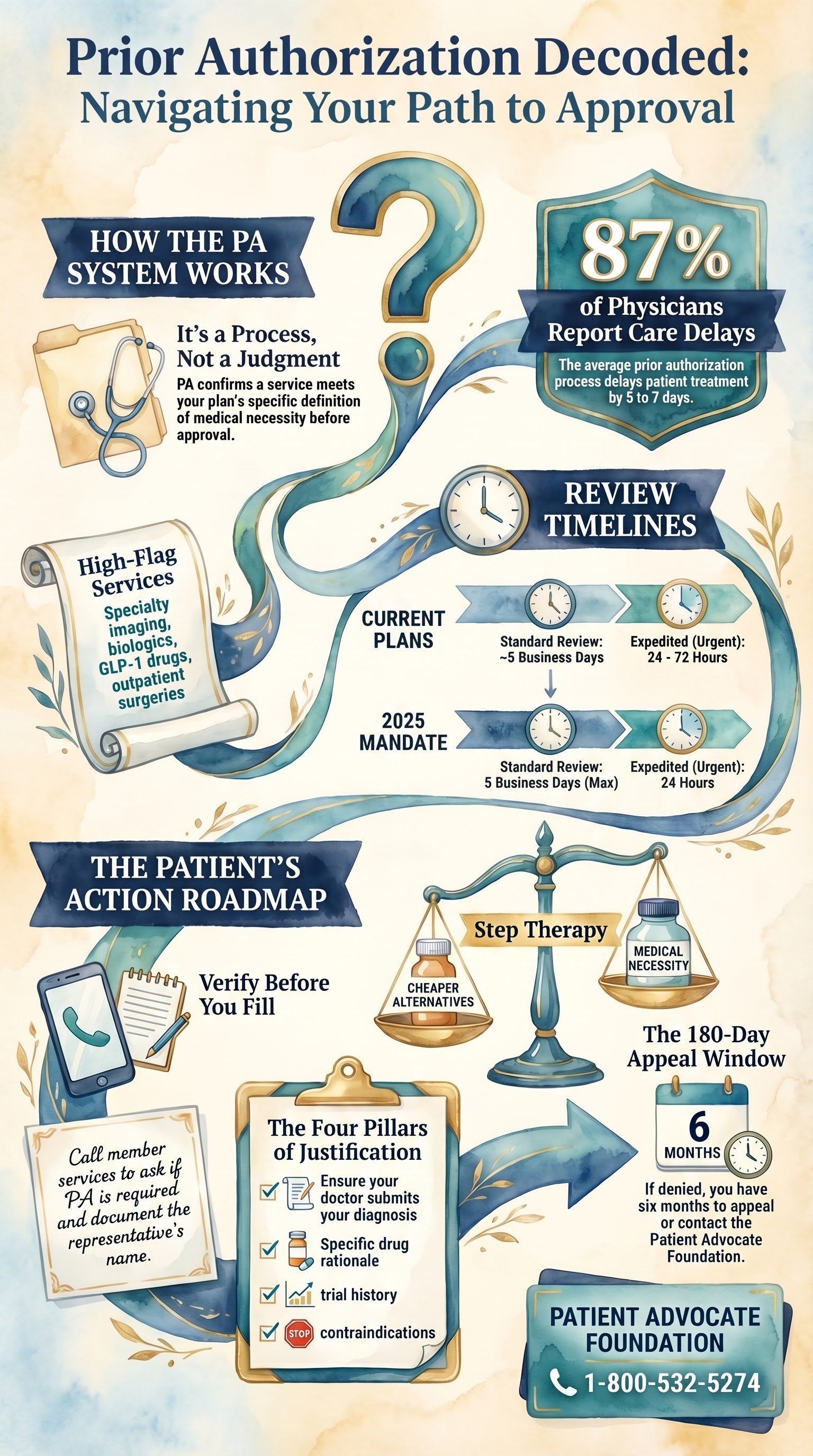
Prior authorization—or PA—is not an insurer’s way of saying no. It’s a process to confirm that a service meets your plan’s definition of medical necessity. Some PAs are approved quickly. Some are denied inappropriately—and yes, that happened to James. But now James (and you) are going to understand how the process works, so you can work it, not just wait for it.
Here’s what PA is, structurally. Your health plan has clinical criteria—rules that define when a service is “medically necessary.” These rules exist for two reasons: cost control (yes, that’s real) and safety (some medicines or procedures need safeguards).
When your doctor prescribes a drug or orders a procedure that your plan has flagged, your insurance doesn’t auto-approve it. Instead, your provider submits a request to the plan’s medical review team. That team looks at three things:
If it does, you get approved—usually within 5 business days. If it doesn’t, you get denied. Here’s the key: a PA denial is not a verdict that you don’t need the drug or procedure. It’s a verdict that the plan thinks it doesn’t meet their criteria. That’s different. And it’s appealable.
Specialty imaging (MRI, CT, PET scans), specialty medications (biologics, GLP-1s, injectable drugs), outpatient surgeries, and some mental health services. Why these? Because they’re high-cost or require clinical justification to rule out cheaper alternatives. In James’s case, a GLP-1 requires PA because his plan wants evidence that he’s tried lifestyle changes first, or cheaper weight-loss drugs first. That’s a real clinical rule—not unreasonable. But how it was applied to James—that’s where the problem happened. And that’s what you need to watch for too.
Here’s the reality of prior authorization right now.
That delay matters. Researchers at Health Affairs found that PA delays treatment by an average of 5–7 days. For acute conditions—infections, acute pain, acute psychiatric crises—5–7 days changes the outcome.
That’s not a complaint—that’s a fact. Your doctor’s office spends time and staff hours submitting PA requests. That’s real cost, and it slows down your care.
PA itself is not evil. Step therapy—requiring you to try a cheaper drug first—makes sense if the cheaper drug is evidence-based. But if you have a contraindication to that cheaper drug, or if you’ve already tried it, a PA denial is wrong. That’s what happened to you. Your plan denied the GLP-1 claiming you hadn’t tried other medications—but you had. The PA documentation from your provider wasn’t clear enough.
Here’s the concrete action plan for James—and for you, starting today:
James will call his plan’s member services (the number is on his insurance card). He’ll say: “I’m about to have [procedure name] or fill [drug name]. Does my plan require prior authorization for this? And if so, what is the specific clinical reason your plan requires PA for this service?” This last question is crucial—James needs to know what his plan is looking for.
Document this conversation. Write down the date, the representative’s name, what they said, and most importantly: the specific PA requirement reason. Why? Because if the PA is denied and James (or you) appeals, you’ll know exactly what the plan said they needed to see.
Ask your doctor’s office to include: (1) your diagnosis, (2) why this specific drug or procedure, (3) what else you’ve already tried, (4) any contraindications or reasons the alternatives won’t work. The more complete the clinical justification, the higher your approval odds.
As of January 2025, Medicare and federally regulated plans must respond to PA requests within 5 business days. If your condition is urgent, you can request an expedited review—they have 24 hours. Ask for expedited review. Don’t accept the standard timeline if you’re in pain or at medical risk.
You have 180 days to appeal. Don’t ignore a denial. Contact your plan’s appeals department, or call the Patient Advocate Foundation at 1–800–532–5274. They provide free help with PA appeals. Next lesson, we’ll walk through the appeal process step by step.
Prior authorization is a process, not a personal judgment. Some PAs are clinically appropriate. Some are inappropriately applied. You can’t control whether your plan approves the PA. But you can control whether your doctor’s office submits complete clinical justification, whether you appeal if denied, and whether you escalate to free resources like the Patient Advocate Foundation. You’re not powerless. You’re informed.
Next lesson: Building Your Case—how to write and submit a strong PA appeal.
Call your prescriber’s office and ask one question: “Has a prior authorization been submitted for my medication, and what clinical documentation did you include?” Write down what they tell you. That single phone call will tell you where your PA actually is in the process.
Build your PA request with the PA Toolkit →This lesson is part of How Your Insurance Actually Works—an evidence-based course designed with clinical expertise by the AnchorWellPress Medical Team. This content is for educational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult your healthcare provider.